DISCLAIMER: Always consult with a healthcare professional before starting any new routines, programs, or nutrition plans to ensure you receive the best medical advice and strategy for your specific individual needs.
Perimenopause and menopause can have a big impact on your family, personal, and social life, work, and day-to-day activities. It often means night sweats, hot flashes, palpitations, trouble sleeping, and headaches and migraines. Itchy skin, poor wound healing, thinning hair, and brittle nails occur frequently. Without estrogen, the salivary glands produce less saliva, increasing your risk for mouth infections, gum problems, and tooth decay. Bone density starts to decrease, making you more susceptible to fractures and injury.
Along with reduced bone density, decreases in muscle strength and mass can impact your flexibility, agility, strength, and mobility. Problems with concentration and memory, feelings of anxiety and depression, mood swings, and irritability are also common. Your risk of menopause complications and health conditions increases as well, including osteoporosis, heart disease, and urinary tract infections.
While many changes occur, which can affect your health, well-being, and quality of life, menopause is not a diagnosis, nor is it a disease. And there are healthful lifestyle changes that you can make to manage the changes it brings.
Cultivating a growth mindset, prioritizing rest, exercise, and a healthy diet, and cutting back on stress are all ways to make menopause easier on your body and brain.
Free Macro Calculator
Personalized to your body, goals, and measurements. You will receive detailed macros for meals, sample day of eating, food selection guidance, hydration + daily supplement suggestions, and more.
How Does Menopause Start?
 Menopause is the point when your ovaries stop releasing eggs and reproductive hormones and you no longer have menstrual periods. The diagnosis of menopause is based on the absence of menstrual bleeding for 12 consecutive months. It is made by reviewing a woman’s symptoms and menstrual and medical history.
Menopause is the point when your ovaries stop releasing eggs and reproductive hormones and you no longer have menstrual periods. The diagnosis of menopause is based on the absence of menstrual bleeding for 12 consecutive months. It is made by reviewing a woman’s symptoms and menstrual and medical history.
Perimenopause is more challenging to diagnose because it is a gradual transition that can last from just a few months to 10 years. It can begin without knowing it or having any menopause-like symptoms. 15 percent of women experience no symptoms, and for those who have, the incidence and severity of symptoms may increase with age (BMC Women Health).
For the majority of women, perimenopause starts in their mid-40s, and the average age at which women in the U.S. reach menopause is 51.
What Does Menopause Feel Like?
Here are a few symptoms that you might experience during menopause.
Hot Flashes

Hot flashes are not only uncomfortable and annoying but aren’t a short-term problem. They can last for many years and some women experience them daily or a few times a week. Hot flashes also vary in severity, from mild to very intense where day-to-day activities cannot be performed.
When a flash happens, you may experience a feeling of heat in your face, neck, arms, and chest. Other symptoms include tingling in your fingers, sweating, rapid heartbeat, anxiety, and chill once the hot flash subsides.
Night Sweats And/Or Cold Flashes

Like hot flashes, night sweats are common during perimenopause and menopause. About 36 percent of women experience them while 6 percent find night sweats to be bothersome, one study found. Frequency varies between women but has been shown to increase significantly at menopause, peaking 1 month before the final menstrual period.
Excessive sweating or perspiration is one symptom that night sweats and hot flashes have in common. These episodes occur during sleep and can be so severe as to wake you up with soaked bedding and sleepwear. Contributing factors include early age at first pregnancy, smoking, diabetes, high-risk drinking, and premenstrual tension (Menopause).
Vaginal Dryness That Causes Discomfort During Sex

Vaginal dryness is a common condition in menopausal women, with 25 to 57 percent reporting dryness and urinary symptoms (Menopause). It is characterized by burning and itching sensations, discomfort and pain during intercourse, and frequent urinary tract infections. Other symptoms include burning with or frequent urination, incontinence, vaginal discharge, and bleeding after intercourse.
At menopause, vaginal dryness is caused by a lack of lubrication due to low levels of estrogen. This drop in reproductive hormones causes the vaginal tissues to thin, leaving fewer cells secreting moisture. Other factors that contribute to dryness in post- and perimenopausal women include inflammatory and metabolic conditions, certain medications, and unhealthy behaviors such as cigarette smoking.
Urinary Incontinence
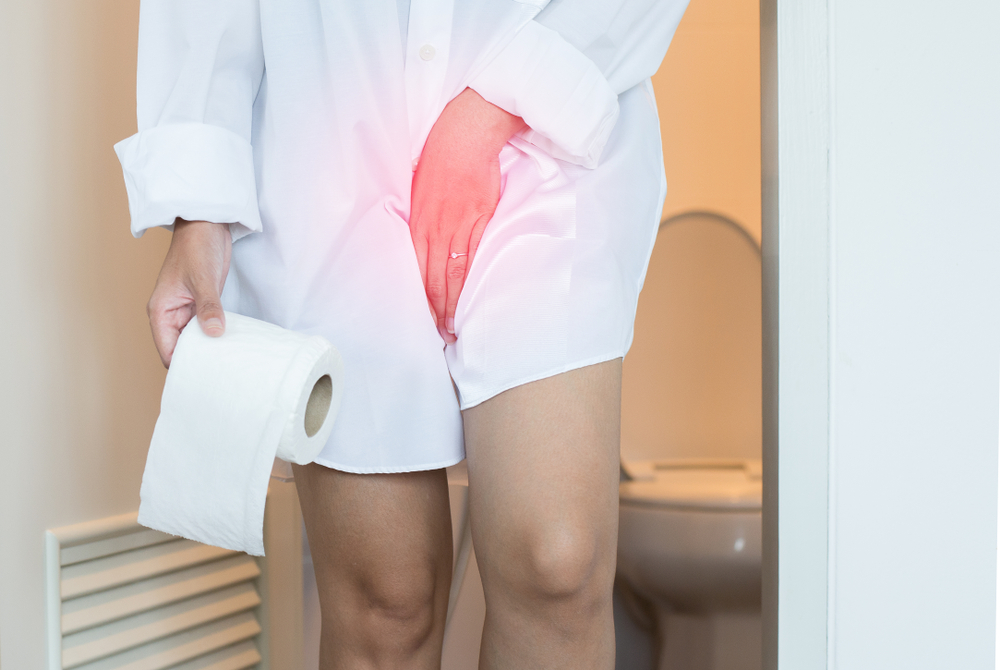
The drop in estrogen near menopause causes the pelvic floor muscles to weaken. When put under strain, the pelvic floor may be unable to prevent urination. Symptoms include leaking urine when coughing, sneezing, lifting heavy, and exercising, pelvic pain, waking up to urinate, and wetting your bed at night.
Insomnia
 While short-term insomnia is often due to a traumatic event or stress, menopause-related sleep disturbances are caused by falling levels of progesterone and estrogen. Depression and anxiety, changes in mood, night sweats, and hot flashes also contribute to frequent waking and poor sleep. Symptoms of insomnia include feeling tired or sleepy during the day, waking up too early, less than 6 hours of sleep at night, and not feeling rested when you wake up.
While short-term insomnia is often due to a traumatic event or stress, menopause-related sleep disturbances are caused by falling levels of progesterone and estrogen. Depression and anxiety, changes in mood, night sweats, and hot flashes also contribute to frequent waking and poor sleep. Symptoms of insomnia include feeling tired or sleepy during the day, waking up too early, less than 6 hours of sleep at night, and not feeling rested when you wake up.
Insomnia can affect your body in several ways such as feeling stressed, irritable, and anxious, having slowed reaction time and poor concentration, and experiencing more accidents and errors. Complications include mood disorders, high blood pressure, diabetes, and heart disease.
Emotional Changes
Declining levels of estrogen can cause a range of emotional symptoms, from mood swings and irritation to depression. Symptoms also include crying, snappiness, bursts of anger, panic attacks, worsening premenstrual tension, and loss of confidence and self-esteem. Some women are at a greater risk of experiencing emotional distress, including those in a difficult living situation or toxic relationship, women under a lot of stress, and those with a history of severe PMS.
Dry Skin, Dry Eyes, Or Dry Mouth

Skin loses collagen during menopause, causing it to dry and age faster. You are likely to find your skin dry just about anywhere, like your legs, elbows, chest, back, and face. Fine wrinkles and dark spots also appear as your skin loses moisture and elasticity.
Menopausal women are more prone to dry eyes as well. While the relationship is unknown, estrogen and androgen, which decline near menopause, may play a role in tear production.
Other factors, including the use of antihistamines, diabetes, and thyroid disease may also contribute to developing dry eye disease. Environmental factors are also known to cause increased tear evaporation, including air conditioning, wind, dry air in winter, and outdoor sports like boating and skiing.
Symptoms of dry eyes include:
– Blurred vision
– Itchy or red eyes
– Burning
– Pain
– Dry or tired eyes
– Light sensitivity
– Visual discomfort
– Gritty feeling in the eyes
Likewise, the exact link between falling levels of reproductive hormones and dry mouth is not well understood. One hypothesis is that the drop in estrogen during menopause causes a reduction in the flow of saliva. When the production of saliva is reduced, this can cause gum disease, tooth decay, soreness and burning sensations, and frequent mouth infections.
Breast Tenderness and Pain

Breast pain or mastalgia affects up to 70 percent of women at different stages of life but is most common in women aged 40 to 50 (Breast Care). Some women experience soreness, burning, or tenderness while others report a throbbing, sharp, or stabbing pain.
Women who are on hormonal therapy or oral contraceptives are more prone to experience cyclical breast pain in the years leading to the onset of menopause (Harvard Health Publishing). Other factors that contribute to breast pain and tenderness at midlife include fibrocystic changes, infections, trauma, and medications like diuretics and psychiatric and cardiovascular drugs.
Worsening of Premenstrual Syndrome (PMS)

Bloating, fatigue, mood swings, breast tenderness, and food cravings are symptoms of PMS that most of us are familiar with. Some women also experience sleep issues, difficulty concentrating, anxiety, sadness, and irritability.
During the transition to menopause, women are more likely to experience PMS symptoms. When you add hot flashes, night sweats, and insomnia, they may feel worse, with women tolerating them less well.
Irregular Periods or Periods That Are Heavier/Lighter Than Usual
As the ovaries begin to produce less estrogen during perimenopause, your cycle may become lighter, heavier, or more irregular or erratic. Irregular periods may be accompanied by vomiting, nausea, cramping, and pain, with spotting or bleeding occurring between periods.
In addition, your cycle can become shorter or longer, and a space of 60 days or more shows that you are likely approaching menopause. You may also skip periods, notice blood clots, or experience changes in the menstrual flow such as clumpy and thick or watery and thin discharge. All these are due to estrogen fluctuations causing irregularities in your menstrual cycle.
Free Macro Calculator
Personalized to your body, goals, and measurements. You will receive detailed macros for meals, sample day of eating, food selection guidance, hydration + daily supplement suggestions, and more.
How to Make Menopausal Changes Less Painful?
Going through menopause is tough enough, so here are a few tips you might find helpful while going through that time.
1. Develop a Growth Mindset

Menopause is a natural stage of a woman’s reproductive cycle. It isn’t something that can be or needs to be fixed but a normal transition in life. If menopausal symptoms are more severe, however, you’ll want to develop a growth mindset as a way to mitigate symptoms.
Challenges, pleasures, and ups and downs are all part of the human experience. Cultivating a positive mindset can also help ease your way through menopause. One study shows that women who view menopause as a positive experience have fewer depressive symptoms and report a more positive body image. A review of 16 studies also found that women with a more positive attitude experience fewer symptoms.
2. Maintain a Healthy Body Weight

Pounds begin to accumulate around your middle once you hit menopause. And excess belly fat isn’t just frustrating but dangerous because it puts you at risk for a range of health conditions like liver problems, diabetes, and cardiovascular disease.
To maintain a healthy weight at menopause, it’s best to focus on a balanced, varied diet that supports weight loss and low body fat. Include lean proteins such as beef, turkey, and chicken which help prevent muscle loss, boost your metabolism, and keep you fuller for longer.
Eat plenty of fruits and vegetables as well, including avocado, pears, raspberries, and broccoli. High-fiber foods reduce hunger and appetite and keep insulin in check. Make sure you consume dairy products as they help the body maintain muscle mass and support weight loss.
3. Prioritize Strength Training and Build Muscle

The risk for osteoporosis increases at menopause, making physical activity an important protective factor. Strength training, in particular, boosts metabolism, enhances muscle mass, supports bone health, and promotes flexibility and mobility. Studies also show that strength training improves insulin sensitivity, decreases blood pressure, and reduces the risk of cardiovascular disease.
With plenty of benefits to your body, if you’ve never done weight training, now it’s a good time to give it a try. Start with exercises that improve core stability and balance, including pulling, pushing, bend-and-lift, and bodyweight squats. Then you can include machines with cables and weights to build muscle mass and strength and improve endurance.
4. Prioritize Rest, Recovery, and Sleep

If you are supporting children, caring for aging parents, and dealing with tight deadlines at work, anxiety, and stress may keep you from sleeping. Add night sweats and hot flashes, and you may find yourself struggling with waking up night after night.
Not getting enough sleep can lead to injuries and falls, sabotaging decision-making and resulting in impaired judgment. An ongoing lack of sleep also increases the risk of anxiety and depression, hypertension, and cardiovascular disease.
To improve your sleep and minimize health risks associated with insomnia, avoid exercise, heavy meals, and caffeine before going to bed. Try not to use your mobile or laptop around bedtime and listen to relaxing music or read a book instead. Stick to a sleep schedule, avoid napping during the day, and make sure your sleeping environment is as relaxing and comfortable as possible.
5. Reduce Stress

The time around menopause is stressful for many women. In addition to troubling symptoms like night sweats, hot flashes, and mood swings, busy work schedules, aging parents, demands of teenage children, and other responsibilities can lead to stress, strain, and responsibility fatigue.
As stress can lead to a ton of health issues, including hypertension and heart disease, you should try to limit the amount of stress in your life. Seek out social support, ask for help when feeling exhausted, and sort out tasks according to priority. Find ways to relax, try yoga, meditation, and music relaxation, and treat yourself to a long bath, manicure, or massage.
Wrapping Up
 Menopause and the symptoms it can bring can hurt your quality of life. Sleep may become elusive, with hot flashes and night sweats leaving you exhausted and low. Many women also experience anxiety, mood swings, brain fog, and a devastating loss of confidence and become socially withdrawn as a result.
Menopause and the symptoms it can bring can hurt your quality of life. Sleep may become elusive, with hot flashes and night sweats leaving you exhausted and low. Many women also experience anxiety, mood swings, brain fog, and a devastating loss of confidence and become socially withdrawn as a result.
As troublesome as your symptoms might be, menopause is not a disorder, and nor is it a disease. As with every new life chapter, the changes menopause brings call for lifestyle modifications. What is to be done? Your old trusty allies, food, exercise, and rest can help. Engage in weight training exercises, eat a balanced, nutrient-rich diet, and be protective of your sleep. Give yourself the love and compassion you need, cultivate a positive mindset, and embrace menopause as a natural stage of aging, with all the pros and cons and good and bad.
Free Macro Calculator
Personalized to your body, goals, and measurements. You will receive detailed macros for meals, sample day of eating, food selection guidance, hydration + daily supplement suggestions, and more.
DISCLAIMER: Always consult with a healthcare professional before starting any new routines, programs, or nutrition plans to ensure you receive the best medical advice and strategy for your specific individual needs.

Terry Tateossian is a Menopause Lifestyle Medicine Coach, Certified Personal Trainer & Nutritionist and the Founder of THOR: The House of Rose, a wellness brand serving women over 40 through retreats, coaching, macro-nutrition and community. As 25-year founder and entrepreneur, Terry spent two and a half decades building and running successful start-up businesses, an experience that put her on the front line of founder burnout long before she could name it. After facing serious health challenges, early onset menopause, and emotional eating while running her agency and raising two children, Terry rebuilt her health in her 40s and lost more than 80 pounds through evidence-based nutrition, training, and mindset work. Today, she helps women get strong, improve confidence, support hormone health, and create a stronger second half of life. Terry has been featured in major media outlets and is available for podcasts, expert commentary, brand collaborations, and speaking engagements on midlife health, reinvention, emotional eating, menopause wellness, and strength training for longevity. Get her free macro calculator (her cookbook companion) to start your journey to back to health.


 By Team THOR
By Team THOR